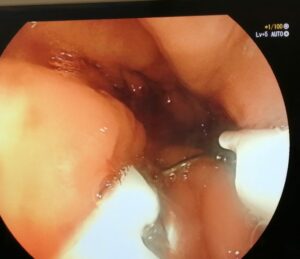
Endoscopic sleeve gastroplasty
endoscopY
The hole procedure through the mouth.
Under anesthesia.
No incision. No scar.

BARIATRIC
Weight loss procedure
19-20% average weight loss
beneficial
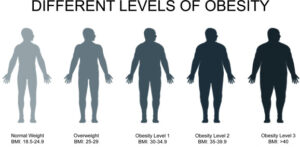
to obese patients (BMI> 30 kg / m2)

LOW invasive
1 hour 15 minutes of intervention
1 night at the clinic
Fast recovery
Exceptional complications
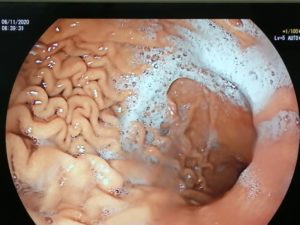
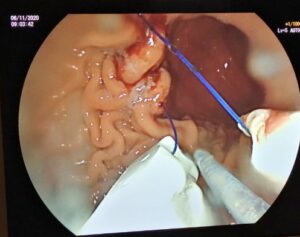
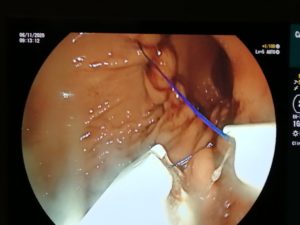
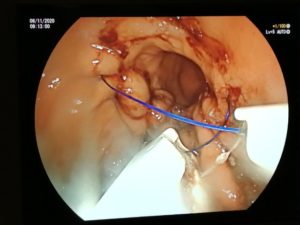
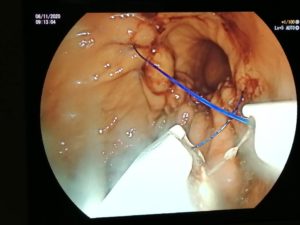
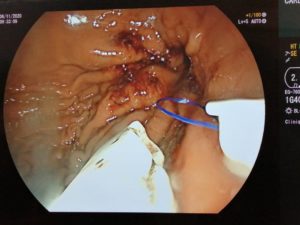
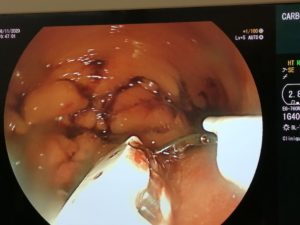
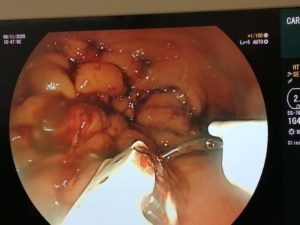
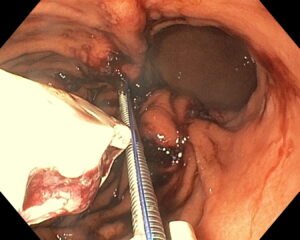
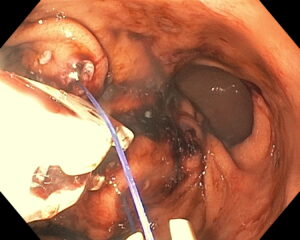
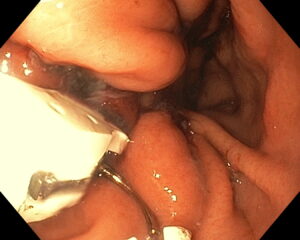
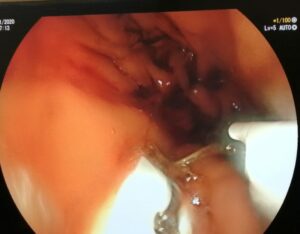
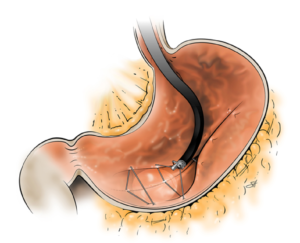
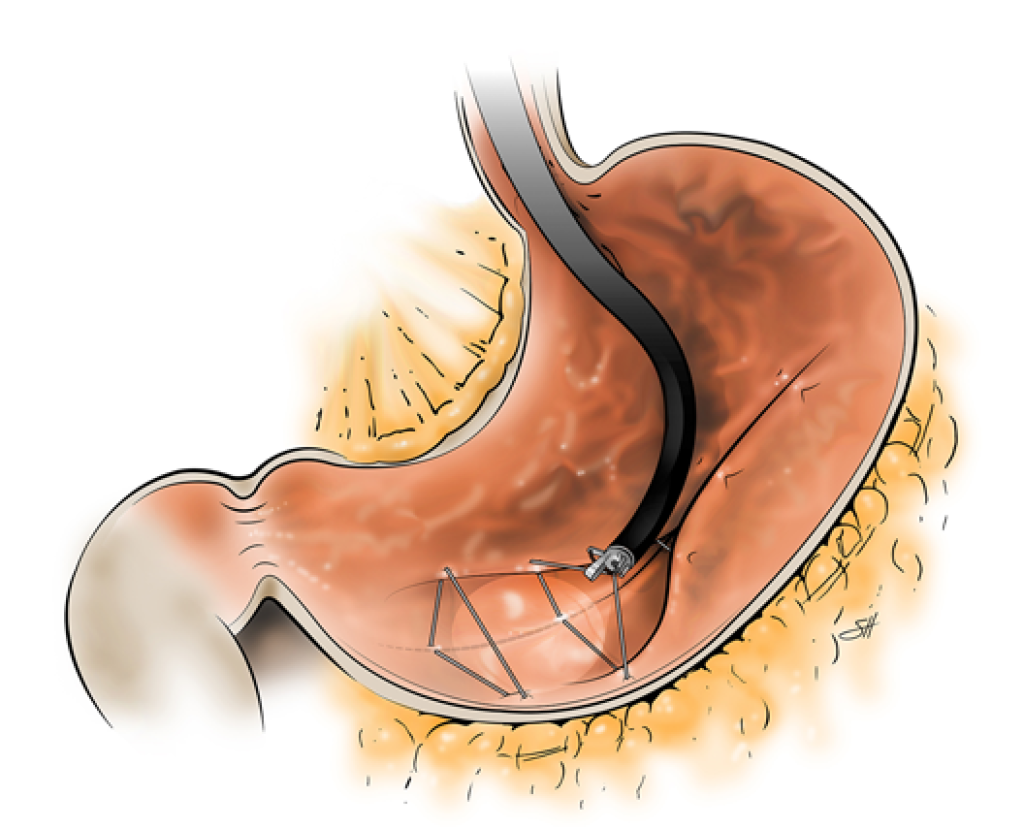
ENDOSCOPIC SLEEVE TECHNIQUE
The size of the stomach is reduced with a series of sutures made in a U-shaped pattern at the walls of the stomach.
By tightening these sutures, the stomach will shrink in size, like an accordion.
This non-surgical technique is performed under general anesthesia without incision, through the mouth.
The procedure lasts around 1 hour 15 minutes.
The video below shows you what the technique involves.
ENDOSCOPIC SLEEVE : FOR WHO ?
IMC : more than 30 kg/m²
The average weight loss after a plication is 20% of the body weight. (results chapter).
Therefore, gastric plication will benefit most patients with a body mass index (BMI) greater than 30, who have failed to maintain weight loss with a single lifestyle modification.
In all cases, the plication must be accompanied by a healthier lifestyle, and dietary monitoring. (chapter monitoring).
Supplied by BMI Calculator USA
FAQ on endoscopic sleeve gastroplasty
How much weight does endoscopic gastric plication makes lose?
The average weight loss is 20% which means some patients will lose less and some will lose more. How much weight you lose will depend in part on how you use this tool, how well you maintain a consistent diet and exercise program, and how often you follow up with your healthcare team.
Some patients regularly lose 25%, 30% or more of their body weight. Although these numbers are above the « average », they are still possible.
Are there any major risks reported? Excessive bleeding or something else that is life threatening ?
There is an approximately 0.5% risk of a serious adverse event, including infection and bleeding. If a complication were to occur, it would be early (within the first 3 days). There are no proven long-term risks. A telephone link is always available in case of serious concern. Although this is not a surgical procedure, it is a procedure and the risks should be taken into account.
Is this procedure reversible? Does the sutured stomach dilate over time and enlarge?
Endoscopic plication is a permanent procedure. Cutting the threads and recovering the initial stomach is feasible but technically difficult. There really isn’t really a medical reason for it to happen.
However, no weight loss procedure can be guaranteed to last forever and the stomach has the ability to stretch over time if a person eats too much or does not stick to the recommended diet.
This is also true in the event of bypass, or surgical sleeve.
Can food or liquids can get trapped behind the suture line??
No. There is actually no space or pocket behind the sutures. Everything closes when the sutures are tightened.
Is endoscopic sleeve gastroplasty feasible in case of hiatal hernia?
Yes, endoscopic sleeve gastroplasty can be performed safely when a small or medium hiatus hernia is present (less than 5 cm).
Les sutures sont-elles permanentes, les patients doivent-ils les faire retirer à l’avenir? Que se passe-t-il si la suture éclate ?
Oui, les fils de suture sont permanents (non solubles). Ils n’ont pas besoin d’être retirés. Si l’un d’entre eux venait à se détacher, cela ne causerait aucun mal.
What is the approximate delay to be operated ?
The lead time is approximately 8 weeks. This period is very important because it includes an information and questioning phase where the patient can ask me all the questions he wants by phone, email or in consultation. There is then a thinking phase, an assessment in a day hospital, a preliminary fibroscopy.
And it’s D-Day!
Can we benefit from an endoscopic gastric plication after having benefited in the past from a surgical sleeve ?
This is not only possible, but if it works very well according to multiple studies. The endoscopic sleeve made it possible to tighten much more the line of staples which would have been stretched over time after a surgical sleeve.
Is the endoscopic gastric plication a competing technique of the surgical sleeve ?
As I said above, endoscopic sleeve gastroplasty induces a 20% total body weight loss, and is consequently intended for patients who have between 15 and 25 kg to lose in general.
These patients have a BMI of between 30 and 37 while surgical techniques are primarily intended for patients with a BMI greater than 40.
As far as I’m concerned, I work hand in hand with surgeons and it is very common that we address patients for whom the techniques of my colleagues are more suitable and vice versa.